Neonatal Intensive Care Unit (NICU)
Focusing on the Most Vulnerable Patients
Home / NICU
NICU
Neonatal Intensive Care Unit (NICU)
Neonatal Intensive Care Unit (NICU)
Focusing on the Most Vulnerable Patients
We have always kept neonatal patients close to our hearts. With Project Stork and the development of SET® Measure-through Motion and Low Perfusion™ pulse oximetry, Masimo solved seemingly unsolvable problems and made a significant impact on neonatal care, helping clinicians reduce the incidence of retinopathy of prematurity (ROP) and improve critical congenital heart disease (CCHD) screening.
Today, Masimo remains dedicated to helping clinicians improve neonatal care through a variety of innovative clinical solutions.
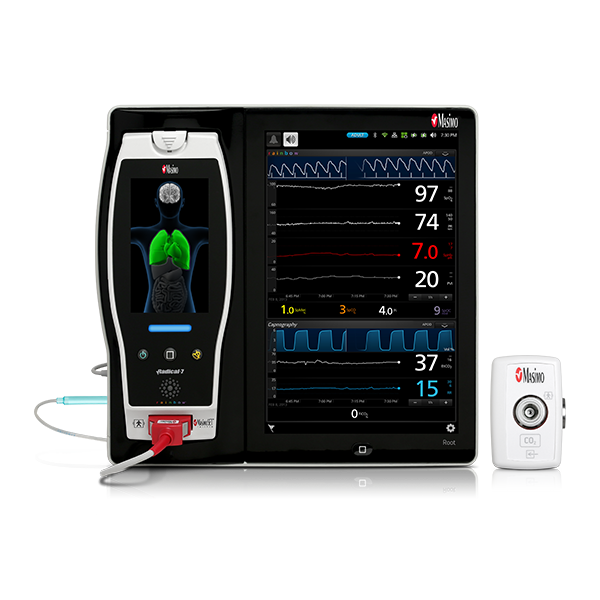
Masimo SET® Measure-through Motion and Low Perfusion™ Pulse Oximetry
Masimo SET® Measure-through Motion and Low Perfusion™ Pulse Oximetry
Masimo’s breakthrough technology, Signal Extraction Technology® (SET®), overcame the limitations of conventional pulse oximetry with the ability to measure through motion and low perfusion. Masimo SET® is able to recognise that both arterial and venous blood can move, using parallel signal processing engines to separate the true arterial signal from sources of noise, including the venous signal. Multiple studies have demonstrated that Masimo SET® outperforms conventional pulse oximetry technologies.1 In one study comparing the ability of three pulse oximetry technologies to detect hypoxic events, Masimo SET® pulse oximetry demonstrated the highest sensitivity and specificity during induced conditions of motion and low perfusion.2
Performance During Motion and Low Perfusion2
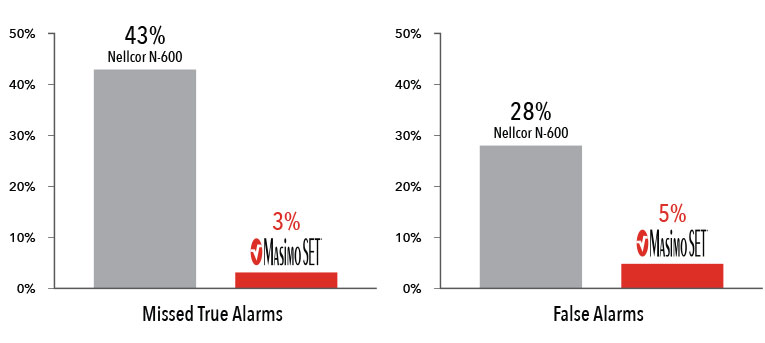
Masimo SET® had 3% missed true alarms and 5% false alarms versus 43% and 28%, respectively, using competitor technology.
Results shown are calculated by combining sensitivity and specificity outcomes of machine-generated and volunteer-generated motion.
At Masimo, innovation never stops. After these studies were published, Masimo achieved significant accuracy specification improvements for RD SET sensors, improving from 3% ARMS to 1.5% ARMS* in conditions of motion.
Reducing Retinopathy of Prematurity (ROP)
Reducing Retinopathy of Prematurity (ROP)
Premature infants in neonatal intensive care units are routinely administered supplemental oxygen to help preserve vital organ function. However, too much oxygen administration, which can lead to hyperoxia, can increase the risk of severe eye damage from retinopathy of prematurity (ROP).3 Clinicians use pulse oximetry to help manage the administration of oxygen, but unreliable pulse oximetry measurements can result in over administration of oxygen and subsequent ROP.
In two NICU settings, Masimo SET® Measure-through Motion and Low Perfusion pulse oximetry, coupled with changes in clinical practice, showed significantly reduced rates of severe retinopathy of prematurity (ROP) and decreased the need for laser therapy.4,5
Severe Retinopathy of Prematurity Rate4
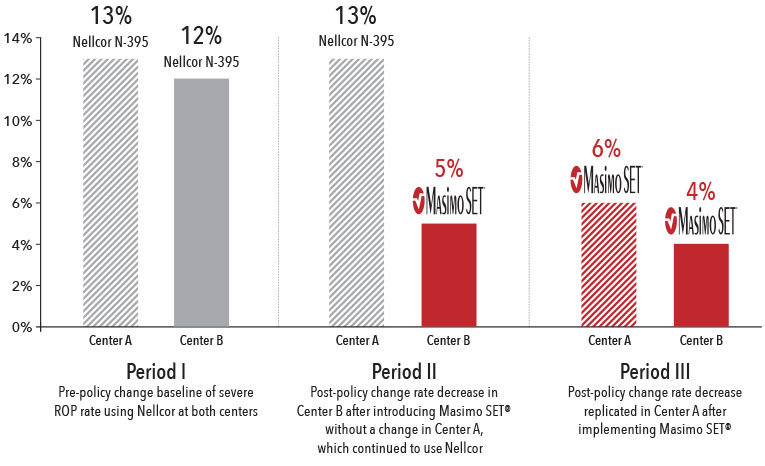
In a study of 571 inborn infants (<1250 g), a change in clinical practice combined with the use of Masimo SET® pulse oximetry led to significant reductions in severe ROP and need for laser therapy.4
Rates of Retinopathy of Prematurity in Very Low Birth Weight Infants5
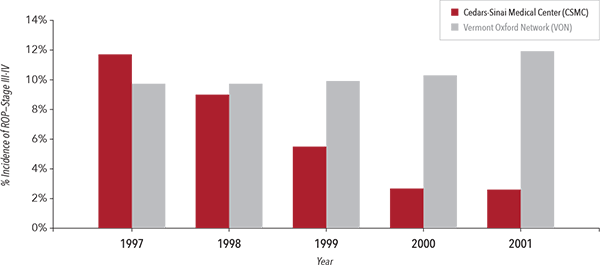
In another study, following the implementation of Masimo SET® with a new protocol in a single tertiary neonatal center at Cedars-Sinai Medical Center (CSMC), the incidence of severe ROP decreased over a five-year period from 12.5% to 2.5% in very low birth weight infants.5
Acquired Methaemoglobinemia
Acquired Methaemoglobinemia
Methaemoglobinemia is a blood disorder characterised by an abnormal amount of methaemoglobin—a form of haemoglobin unable to effectively bind to oxygen—in the blood. Many drugs commonly used in hospitals—such as lidocaine, benzocaine, dapsone, and nitrates—may cause a dangerous reaction known as acquired methaemoglobinemia.6 Inhaled nitric oxide (iNO) therapy, and even topical anesthetics containing benzocaine or prilocaine, can cause elevated levels of methaemoglobin in neonates and infants.7,8
Masimo Pulse CO-Oximetry provides a method of noninvasively and continuously monitoring methaemoglobin, SpMet®. Real-time SpMet monitoring may help clinicians intervene quickly and appropriately in cases involving elevated methaemoglobin levels.9
Sensors Designed for Neonatal Patients
Capnography Solutions
Capnography Solutions
Masimo offers a portfolio of sidestream capnography solutions to meet the challenges of ventilation monitoring in the NICU. Sidestream CO2 monitoring works with a full family of NomoLine® sampling lines, airway adapter sets, and cannulas for use in a variety of clinical scenarios, including intubated and non-intubated patients in both low and high humidity applications. NomoLine technology is designed for low-flow applications, with a very low sampling rate of 50 ml/min, supporting use on patients with low tidal volumes and high breath rates, common characteristics of neonatal patients. Masimo capnography seamlessly integrates with Masimo SET® pulse oximetry and other key physiologic parameters, providing clinicians with greater visibility to a patient’s oxygenation, ventilation, and respiratory status.
Measurements
Measurements
Products
References:
- 1.
Masimo. Clinical Evidence. https://www.masimo.com/evidence/featured-studies/feature/.
- 2.
Shah et al. J Clin Anesth. 2012;24(5):385-91.
- 3.
Saugstad et al. Journal of Perinatal Medicine. May 2006.
- 4.
Castillo et al. Prevention of retinopathy of prematurity in preterm infants through changes in clinical practice and SpO2 Technology. Acta Paediatr. 2011;100(2):188-92.
- 5.
Chow et al. Can changes in clinical practice decrease the incidence of sever retinopathy of prematurity in very low birth weight infants? Pediatrics. 2003;111(2):339-345.
- 6.
Ash-Bernal R et al. Medicine (Baltimore). 2004;83(5):265-73.
- 7.
Riou Y et al. Pediatric Research. 1998;43:295.
- 8.
U.S. Food & Drug, Consumer Updates, Benzocaine and Babies: Not a Good Mix.
- 9.
Annabi EH et al. Anesth Analg. 2009;108(3):898-9.
- 10.
Yu Y et al. J Biomed Res. 2016;30(1):1-4.
- 11.
Greenberg SB et al. J Crit Care. 2013;28(3):270-6.
*ARMS accuracy is a statistical calculation of the difference between device measurements and reference measurements. Approximately two-thirds of the device measurements fell within ± ARMS of the reference measurements in a controlled study.
RESOURCES
The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
SpMet monitoring is not intended to replace laboratory blood testing. Blood samples should be analyzed by laboratory instruments prior to clinical decision making.
Caution: Federal (USA) law restricts this device to sale by or on the order of a physician. See instructions for use for full prescribing information, including indications, contraindications, warnings, and precautions.
PLCO-004389/PLM-11360B-1220