Med-Surg
Helping Improve Safety and Clinical Efficiencies on the Medical-Surgical Unit
Home / Med-Surg
Med-Surg
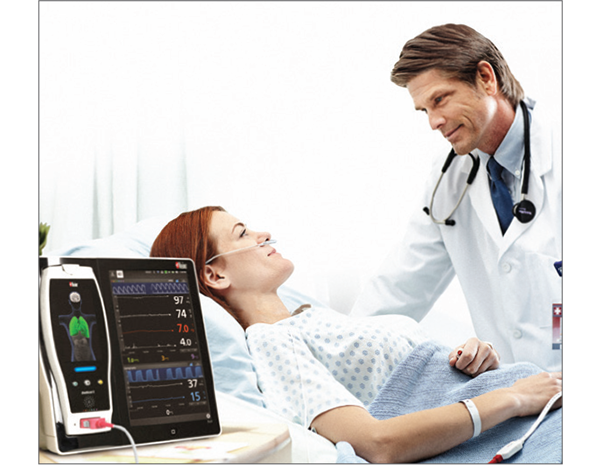
Medical-surgical units are challenged by low nurse-to-patient ratios, increasing case complexity and variability. Clinicians have long understood the value of monitoring in helping to alleviate these burdens, but previous solutions for this environment have been intermittent, delayed and/or limited in their effectiveness. Masimo has developed integrated monitoring technologies providing noninvasive and continuous measurements that automate and streamline the flow of patient data to improve clinical efficiency.
The ability to continuously monitor active patients in medical-surgical units reliably – and to save clinicians’ time by documenting important physiological measurements in electronic medical records – allows clinicians to spend more time caring for patients.
Masimo offers an integrated portfolio of solutions designed to help clinicians focus on patients and improve workflows, including industry-leading SET® pulse oximetry, advanced measurement capabilities, vital signs monitors, portable monitoring devices, and a robust remote monitoring and clinician notification system.
Advancing Patient Safety
Advancing Patient Safety
The Challenges of Alarm Fatigue
Clinicians rely on patient monitors to alert them of adverse changes in a patient’s condition. Alarm fatigue – the sensory overload of an excessive number of alarms – can, however, result in desensitization to alarms and missed alarms, as well as patient discomfort.
Masimo SET® Measure-through Motion and Low Perfusion™ Pulse Oximetry
Masimo’s breakthrough Signal Extraction Technology® (SET®) overcomes the limitations of conventional pulse oximetry with the ability to measure through motion and low perfusion.
Two separate studies found that Masimo SET® pulse oximeters detected approximately 10 times more true events than other "Next Generation" pulse oximeters studied.1,2
Performance During Motion and Low Perfusion3
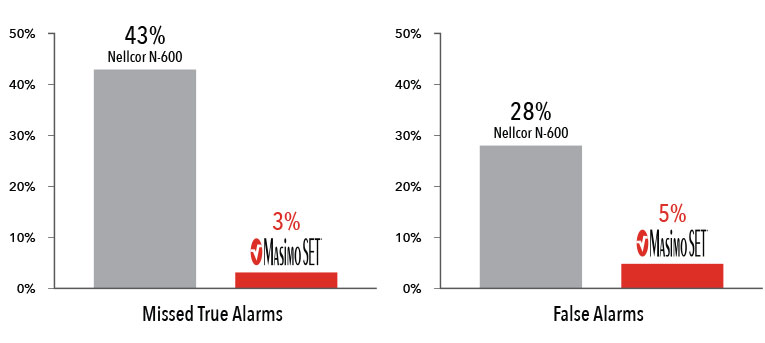
Masimo SET® had 3% missed true alarms and 5% false alarms versus 43% and 28%, respectively, using competitor technology.3
Results shown are calculated by combining sensitivity and specificity outcomes of machine-generated and volunteer-generated motion.
In another study which compared the ability of three pulse oximetry technologies to detect hypoxic events, Masimo SET® pulse oximetry demonstrated the highest sensitivity and specificity during induced conditions of motion and low perfusion.3
Helping Improve Outcomes in Medical-Surgical Units with Patient SafetyNet
In an 11-month study conducted at Dartmouth-Hitchcock Medical Center, Dr. Andreas Taenzer and colleagues found that using Masimo Patient SafetyNet™* and Masimo SET® pulse oximetry as part of a comprehensive alarm management strategy reduced rescue events by 65% and intensive care unit transfers by 48%, and as a result, reduced costs by $1,480,000.4,5 In a subsequent article, they announced that after five years, Dartmouth-Hitchcock had had zero preventable deaths or instances of brain damage due to opioids since the installation of Patient SafetyNet.5 In 2016, after ten years, they reported achieving a 50% reduction in unplanned ICU transfers and a 60% reduction in rescue events, despite increases in patient acuity and occupancy.6
Promoting Efficiency and Versatility
Promoting Efficiency and Versatility
Noninvasive Real-time Measurements
Masimo technology includes a host of noninvasive measurements offered through many patient monitoring solutions, enabling care areas such as the medical-surgical unit, which cater to a variety of patient cases and populations, to customize the type and degree of monitoring needed.
- The rainbow SET™ upgradable technology platform provides measurements and physiologic parameters such as total hemoglobin (SpHb®), carboxyhemoglobin (SpCO®), methemoglobin (SpMet®), and oxygen content (SpOC™) to provide deeper insight into a patient’s status.
- rainbow Acoustic Monitoring® enables monitoring of respiration rate utilizing the unique vibrations associated with breathing for a patient-tolerant7 alternative to capnography.
- NomoLine™ sidestream capnography and gas monitoring provides integrated ventilation monitoring with a wide variety of sampling lines for both intubated and non-intubated patients.
- Noninvasive blood pressure and temperature are integrated into multiple Masimo monitors, offering comprehensive vital signs monitoring, including quick spot-checking during rounds when using optional roll stands.
- Early Warning Score (EWS) calculations provide greater insight into patient status, arming clinicians with more information to help make appropriate care decisions.8
Innovations in Respiration Rate Monitoring: rainbow Acoustic Monitoring®
The Anesthesia Patient Safety Foundation (APSF)9 and The Joint Commission recommend continuous oxygenation and/or ventilation monitoring for patients receiving opioid-based pain medications.10 However, current methods of respiration rate monitoring may be limited by shortcomings related to accuracy and patient tolerance.11,12 rainbow Acoustic Monitoring provides a noninvasive, continuous, easy-to-use, and reliable monitoring solution that has the benefit of higher patient tolerance.13,14
Continuous Monitoring Solutions
Continuous Monitoring Solutions

Masimo offers a portfolio of expandable and configurable patient monitoring solutions designed to adapt to changing patient needs.
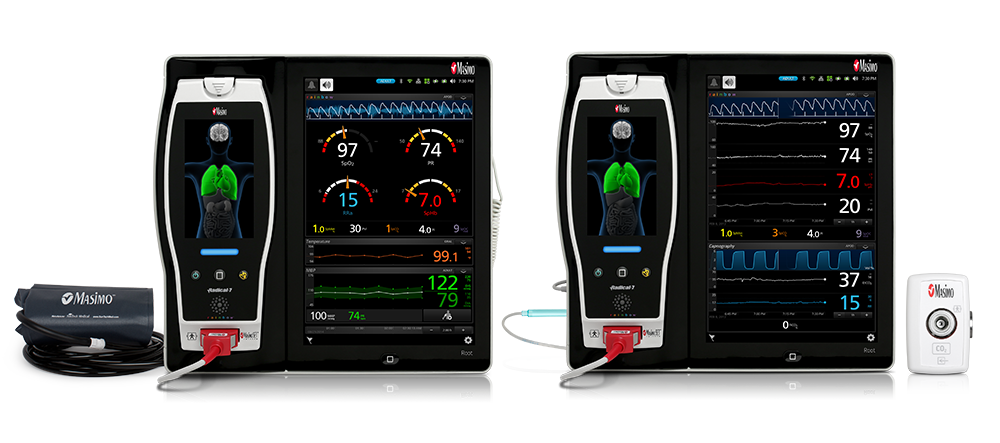
Root with noninvasive blood pressure and temperature and Root with NomoLine capnography. The flexibility and expandability of the Root platform make it an ideal bedside solution, tailorable for both high- and low-acuity settings.
Root® is a powerful, expandable patient monitoring and connectivity hub that integrates an array of technologies to provide multimodal monitoring and connectivity solutions – in a single, clinician-centric platform that allows clinicians to tailor monitoring solutions for high- and low-acuity settings. Root’s plug-and-play expansion capabilities, as well as its availability in a configuration with integrated noninvasive blood pressure and temperature, allow clinicians to centralize patient monitoring by bringing together advanced rainbow SET™ Pulse CO-Oximetry, vital signs measurements, brain function monitoring, regional oximetry, and capnography measurements on an easy-to-interpret, customizable display, empowering clinicians with more information. Further, Root serves as a central connectivity hub, with automated electronic charting of Masimo and third-party device data and alarms to electronic medical record (EMR) systems, which may improve clinician workflows through the reduction of manual data documentation.
Device Integration
Root has the unique ability to bring together data and alarms from multiple third-party monitors — such as IV pumps, ventilators, and other multi-parameter monitors — automating the flow of patient data to the EMR, which may help streamline workflows, improve productivity, and reduce the likelihood of transcription errors.15
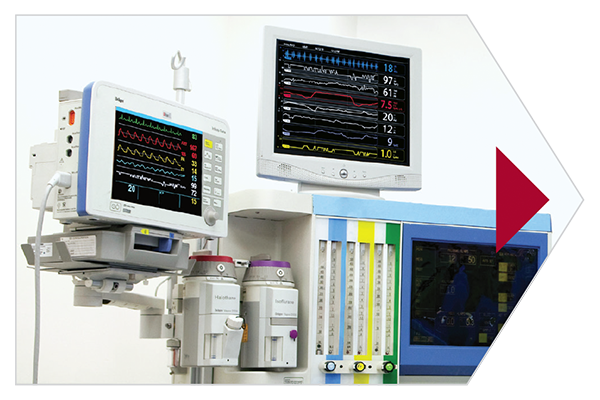
Third-party Devices
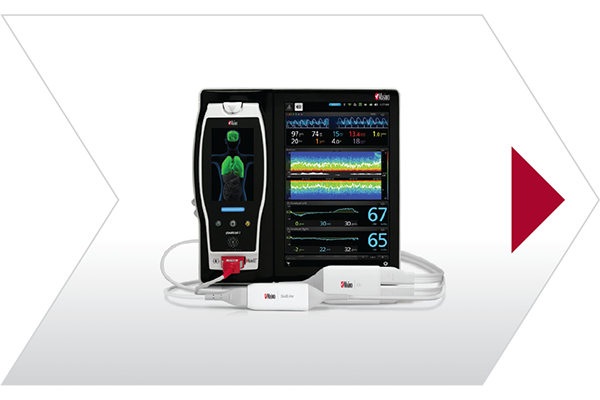
Root

Server

Electronic Medical Record
Bedside Patient Association to Facilitate Positive Patient Association

Used in conjunction with Patient SafetyNet or Iris Gateway™, Clinicians receive ADT information directly on Root, facilitating positive patient identification. Clinicians simply select a patient from a drop-down list or scan the patient’s wristband using an optional barcode scanner, attached to Root, to associate the patient, device, and clinician at the bedside.
The Radius-7® Pulse CO-Oximeter® is a Bluetooth®-enabled wearable monitor used in conjunction with the Root patient monitoring and connectivity platform. Radius-7 provides continuous tetherless monitoring so that patients can ambulate throughout the hospital and have freedom of movement while being continuously monitored. Two "hot-swappable," rechargeable modules with up to 12-hour battery life minimize monitoring interruption and require just one module exchange per shift. The use of single-patient-use armbands minimizes the risk of patient cross contamination.

Flexible, Efficient Spot-checking
Flexible, Efficient Spot-checking

Masimo offers a variety of spot-check and vital signs measurement solutions, allowing facilities to select the best options for their patient needs and workflows.
Root and Root with noninvasive blood pressure and temperature can be mounted on a mobile roll stand, simplifying workflows by facilitating quick vital signs spot-checking and automatically documenting measurements in electronic medical records during rounds.15 Noninvasive blood pressure technology provides three oscillometric blood pressure measurement modes: spot-check, automatic interval, and stat interval. Accessories include both disposable and reusable cuffs for adult, pediatric, and neonatal patients.
Root also includes a number of additional features, such as the ability to connect to and serve as a hub for third-party devices and the ability to calculate an Early Warning Score (EWS) on demand, allowing clinicians to tailor monitoring to best suit a variety of clinical needs.
Simplifying Workflows with Connectivity Solutions
Simplifying Workflows with Connectivity Solutions
Supplemental Remote Monitoring
Masimo Patient SafetyNet optimizes patient safety and clinician workflows through centralized, supplemental remote monitoring and automated charting. Near real-time information from any connected Masimo device, as well as supported third-party devices such as ventilators, is displayed at a central view station, allowing clinicians to quickly assess the status of up to 200 patients, review trend data, and investigate alarms.
When changes occur in measured values, which may indicate deterioration in a patient's condition, Patient SafetyNet automatically sends wireless alerts directly to clinicians, wherever they may be. In addition, Patient SafetyNet can automate the transfer of patient data, vital signs, early warning scores (EWS), and other physiological parameters directly to hospital electronic medical record (EMR) systems, helping to improve clinician workflows and reduce the possibility of transcription errors.15
Escalation Management — Actionable patient alarm notifications are sent to designated clinicians, with automatic escalation, facilitating immediate patient intervention.
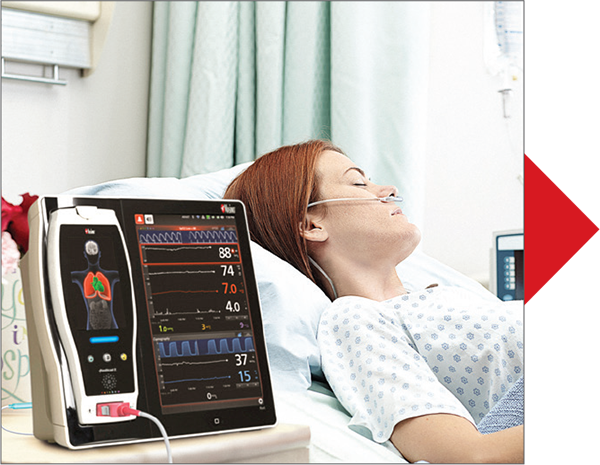
Configure alarm thresholds and delays by patient population to manage alarms

Clinician is notified remotely of alarm at the bedside
If primary clinician does not respond, the alert is escalated to additional clinicians
Device Connectivity
Masimo’s unique approach to device connectivity leverages existing hardware and infrastructure to reduce the cost of connectivity. Iris Gateway and Patient SafetyNet connect Masimo and third-party medical devices’ data and alarms to provide streamlined and cost-effective meaningful use of EMR systems.
Measurements
Measurements
Products
References:
- 1.
Hay WW. Reliability of conventional and new oximetry in neonatal patients. J of Perinatol, 2002;22:360-36.
- 2.
Barker SJ. "Motion-Resistant" Pulse Oximetry: A comparison of new and old models. Anesth Analg. 2002;95(4):967-72.
- 3.
Shah et al. J Clin Anesth. 2012;24(5):385-91.
- 4.
Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
- 5.
Taenzer AH et al. Postoperative Monitoring - The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
- 6.
McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
- 7.
Patino M. et al. Paediatr Anaesth. 2013 Sep 3.
- 8.
As a default, EWS on Root is aligned with the NEWS system established by the Royal College of Physicians using seven (7) physiological contributors as the basis of the scoring system. Royal College of Physicians. National Early Warning Score (NEWS): Standardizing the assessment of acute illness severity in the NHS. Report of a working party. London: RCP, 2012
- 9.
Weinger MB, et al. APSF Newsletter. 2011;26(2):21-40.
- 10.
The Joint Commission Sentinel Event Alert. Issue 49, August 8, 2012. http://www.jointcommission.org/assets/1/18/ SEA_49_opioids_8_2_12_final.pdf
- 11.
Ramsay MAE et al. The accuracy, precision and reliability of measuring ventilatory rate and detecting ventilatory pause by rainbow acoustic monitoring and capnometry. Anesth Analg. 2013 Jul;117(1):69-75.
- 12.
Applegate RA et al. Advanced Monitoring Is Associated with Fewer Alarm Events During Planned Moderate Procedure-Related Sedation: A 2-Part Pilot Trial. Anesth Analg. 2016;122(4):1070-8.
- 13.
Macknet MR et al. Accuracy and Tolerance of a Novel Bioacoustic Respiratory Sensor in Pediatric Patients. Anesthesiology. 2007;107:A84. (abstract).
- 14.
Goudra BG et al. Comparison of Acoustic Respiration Rate, Impedance Pneumography and Capnometry Monitors for Respiration Rate Accuracy and Apnea Detection during GI Endoscopy Anesthesia. Open J Anesthesiol. 2013; 3:74-79.
- 15.
The Value of Medical Device Interoperability. West Health Institute. 2013.
*The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
RESOURCES
Caution: Federal (USA) law restricts this device to sale by or on the order of a physician. See instructions for use for full prescribing information, including indications, contraindications, warnings, and precautions.
The Bluetooth® word mark and logos are registered trademarks owned by Bluetooth® SIG, Inc. and any use of such marks by Masimo is under license.
PLCO-001693/PLM-11088B-0218